Connect With Us

Diabetic Foot Care
Diabetes can cause two problems that can potentially affect the feet: Diabetic neuropathy and Peripheral Vascular Disease. Diabetic neuropathy occurs when nerves in your legs and feet become damaged, which prevents you from feeling heat, cold, or pain. The problem with diabetic neuropathy is that a cut or sore on the foot may go unnoticed and the cut may eventually become infected. This condition is also a main cause of foot ulcers. Additionally, Peripheral vascular disease also affects blood flow in the body. Poor blood flow will cause sores and cuts to take longer to heal. Infections that don’t heal do to poor blood flow can potentially cause ulcers or gangrene.
There are certain foot problems that are more commonly found in people with diabetes such as Athlete’s foot, calluses, corns, blisters, bunions, foot ulcers, ingrown toenails, and plantar warts. These conditions can lead to infection and serious complications such as amputation. Fortunately, proper foot care can help prevent these foot problems before they progress into more serious complications.
Each day you should wash your feet in warm water with a mild soap. When you finish washing your feet, dry them carefully especially between your toes. You should also perform daily foot inspections to ensure you don’t have any redness, blisters, or calluses. Furthermore, if you are diabetic, you should always wear closed-toed shoes or slippers to protect your feet. Practicing these tips will help ensure that your feet are kept healthy and away from infection.
If you have diabetes, contact your podiatrist if you have any of the following symptoms on your feet: changes in skin color, corns or calluses, open sores that are slow to heal, unusual and persistent odor, or changes in skin temperature. Your podiatrist will do a thorough examination of your feet to help treat these problematic conditions.
How Yoga Stretches Can Help Flat Feet

Flat feet, also known as fallen arches, is a condition where the arch of the foot collapses, causing the entire sole to make contact with the ground. This can lead to discomfort, pain, and increased risk of other foot and joint problems. The condition can be caused by genetics, injury, or conditions such as obesity or aging. Yoga can be an effective way to relieve the discomfort caused by flat feet. Specific stretches help strengthen the muscles of the feet and lower legs, improving support for the arch. Poses such as downward dog, warrior 1, and tree pose focus on enhancing foot stability and flexibility. Additionally, yoga promotes proper alignment and body awareness, which can reduce the strain on the feet and prevent further complications. Regular yoga practice can improve overall foot strength and flexibility, providing relief and potentially preventing the progression of flat feet. If you have flat feet, it is suggested that you are under the care of a podiatrist who can offer effective relief tips, which can include specific yoga stretches.
Stretching the feet is a great way to prevent injuries. If you have any concerns with your feet consult with Daniel Bell, DPM from Florida. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
Stretching the Feet
Stretching the muscles in the foot is an important part in any physical activity. Feet that are tight can lead to less flexibility and make you more prone to injury. One of the most common forms of foot pain, plantar fasciitis, can be stretched out to help ease the pain. Stretching can not only ease pain from plantar fasciitis but also prevent it as well. However, it is important to see a podiatrist first if stretching is right for you. Podiatrists can also recommend other ways to stretch your feet. Once you know whether stretching is right for you, here are some excellent stretches you can do.
- Using a foam roller or any cylindrical object (a water bottle or soda can will do), roll the object under your foot back and forth. You should also exert pressure on the object. Be sure to do this to both feet for a minute. Do this exercise three times each.
- Similar to the previous one, take a ball, such as a tennis ball, and roll it under your foot while seated and exert pressure on it.
- Grab a resistance band or towel and take a seat. If you are using a towel, fold it length wise. Next put either one between the ball of your foot and heel and pull with both hands on each side towards you. Hold this for 15 seconds and then switch feet. Do this three times for each foot.
- Finally hold your big toe while crossing one leg over the other. Pull the toe towards you and hold for 15 seconds. Once again do this three times per foot.
It is best to go easy when first stretching your foot and work your way up. If your foot starts hurting, stop exercising and ice and rest the foot. It is advised to then see a podiatrist for help.
If you have any questions, please feel free to contact our office located in Pembroke Pines and Plantation, FL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
How to Stretch Your Feet
Your feet endure a great amount of stress each day from constantly allowing us to move around. It is important to stretch your feet to help prevent them from becoming injured. Your toes may easily deform into unhealthful positions if they are not stretched.
One of the most common reasons for toe deformities are the shoes you may be wearing. Shoes that are too tight may fold and shift the toes out of place. Heeled shoes may also push your toes upward. Forcing your toes into an unnatural position which may cause the muscles to tighten and prevent them from reverting to normal length. Another common reason is improper use of foot muscles. Many people fail to use the muscles in their feet or toes when they walk. Lastly, the positioning of your feet while walking may also cause toe deformities. If you walk with your feet facing outward, your “push-off” phase is on the side of your big toe instead of the bottom of your foot. This may cause the big toe to eventually tighten into a new shifted position.
There are many reasons why stretching your toes may be helpful. One reason is that healthy spacing may aid in avoiding calluses and other injuries that are caused by rubbing. Stretching will also prevent you from developing toes that curl, hammertoes, or bunions.
A great way to stretch your toes is to place them in your hands and bend them all downward; this will help you stretch the top of your foot. Next, you should repeat this process but instead bend them upward enough to feel a nice stretch in the bottom of your foot. You should then try to pull each toe apart from the next and pull any toes that are bent upward until they are back downward.
If you are looking to practice stretching your entire foot, you can try a towel stretch. This is done by sitting on the floor with your legs in front of you. Take a towel and wrap it around your toes. Afterward, pull the towel toward you with your toes and hold this position for 15 to 30 seconds before releasing. Practice this stretch for three sets. Another stretch your feet are towel lifts. This is done by sitting in a chair and trying to pick a towel up from the ground with your toes. Try lifting the towel with your little toes for five sets before switching feet.
If you are an athlete, or exercise often, it is especially important for you to practice stretching your feet. Those who suffer from foot pain caused by poor footwear, plantar fasciitis, or long hours of standing at work may also benefit from foot exercises.
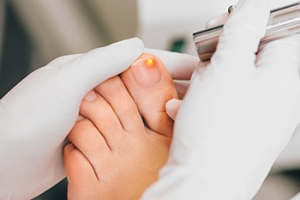
Onychomycosis and the Effectiveness of Laser Treatment
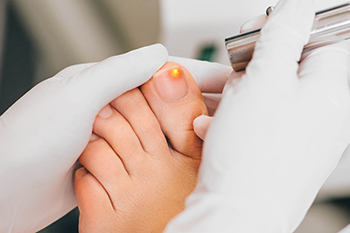
Onychomycosis is a fungal infection that causes the nails to become discolored, thickened, and brittle. This condition is commonly found in toenails but can also affect fingernails. The infection occurs when fungi, typically dermatophytes, invade the nail bed leading to visible damage. Traditional treatments for onychomycosis include antifungal creams and oral medications, but they may take time or have side effects. Laser treatment has become an effective alternative, as it uses targeted light to penetrate the nail and destroy the fungus without harming surrounding tissue. The heat from the laser kills the fungal cells, promoting healing and reducing the risk of recurrence. Laser treatment for onychomycosis is generally safe, with minimal side effects, and can offer quicker results than n other treatments, making it a popular choice for those seeking relief from this persistent condition. If you have developed toenail fungus, it is suggested that you contact a podiatrist who can discuss whether laser treatment is right for you.
Laser treatment can be an effective way to get rid of toenail fungus. If you have any questions about laser treatment, consult with Daniel Bell, DPM from Florida. Our doctor will assess your condition and provide you with quality treatment for fungal nails.
What Are Toenail Fungal Infections?
Onychomycosis, or fungal infection of the nail, is a relatively common and non-serious condition. Around 10 percent of U.S. citizens are afflicted with fungal nails. Common forms of fungus that infect the nail include dermatophytes, yeasts, and molds.
Symptoms of Toenail Fungal Infections Include:
- Nail thickening
- Brittleness of the nail
- Discoloration of the nail
Diagnosis for Fungal Nails
Fungal infections are diagnosed by fungal culture and microscopy. This will rule out any other conditions such as nail trauma, psoriasis, lichen planus, and onychogryphosis.
What Is Laser Treatment?
Laser treatment is a non-invasive, safe, quick, and painless procedure that uses the heat from a laser to kill fungus in the nail. Each infected nail is targeted with a laser for several minutes. The treatment is usually utilized several different times over a select period. During this time, a podiatrist will keep an eye on the infection.
If you have any questions, please feel free to contact our office located in Pembroke Pines and Plantation, FL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Laser Treatment for Fungal Nails
A new treatment for fungal nails, or onychomycosis, which has grown in popularity in recent years, is laser treatment. Laser treatment involves the use of a laser that kills fungus in the toenail with heat. Laser therapy causes no side effects and does not affect nearby healthy tissue.
Toenail fungus afflicts almost 10 percent of the U.S. population and is more common among the elderly. The most common symptom of toenail fungus is the discoloration and thickening of the nail. The nail can also become brittle and a foul smell may be produced. In rare cases, pain might be present. While it is not a serious condition, it can lead to a perception of disgust amongst those it affects. There are several different fungi that cause fungal infections. These include dermatophyte, yeast, and mold. The most common of these is dermatophyte.
Diagnosis for fungal nails involves a podiatrist utilizing microscopy and fungal cultures. This will allow the doctor to determine whether it is a fungus or another condition, such as lichen planus, psoriasis, nail damage, and onychogryphosis.
Fungus in the nails can be hard to get rid of with over-the-counter drugs. This is due to the nail being hard and protective, with fungus able to slip between the nail bed and plate. Furthermore the slow growth of the nail increases the difficulty of fungus going away. Laser treatment seeks to get around this by directly penetrating through the nail and killing the fungus. The laser is used on each infected nail for a couple of minutes. Patients then typically return several weeks or months later for another laser treatment. During this time the podiatrist will routinely observe the foot and infection. It is also recommended to wear clean socks and shoes and allow the feet to dry and breathe to prevent toenail fungus.
Laser treatment is still a relatively new treatment and not all podiatrists have laser machines. Ask your podiatrist if they do laser treatment for toenail fungus and if it is right for you.
See Your Foot Specialist Regularly If You Work On Your Feet
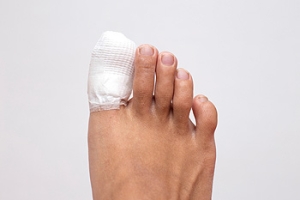
Healing Toe Fractures
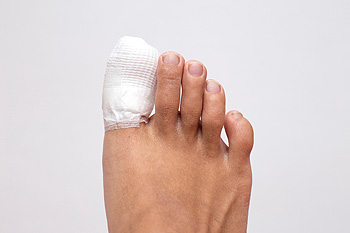
Returning to your favorite sport after a toe fracture requires patience and care. Whether it is an acute injury or a stress fracture, the healing process depends on resting and avoiding pressure on the affected toe. Gradually reintroduce weight-bearing activities as your pain decreases and mobility improves. Wearing supportive footwear with stiff soles or custom orthotics can reduce stress on the toe during recovery. Stretching and strengthening exercises help restore range of motion and prevent stiffness. Overdoing it can delay healing. Always listen to your body as pain is a signal to back off. Before jumping back into full activity, it is suggested that you consult a podiatrist to ensure proper alignment and healing. They can guide you on the safest way to return to play, so you avoid setbacks or reinjury.
A broken toe can be very painful and lead to complications if not properly fixed. If you have any concerns about your feet, contact Daniel Bell, DPM from Florida. Our doctor will treat your foot and ankle needs.
What to Know About a Broken Toe
Although most people try to avoid foot trauma such as banging, stubbing, or dropping heavy objects on their feet, the unfortunate fact is that it is a common occurrence. Given the fact that toes are positioned in front of the feet, they typically sustain the brunt of such trauma. When trauma occurs to a toe, the result can be a painful break (fracture).
Symptoms of a Broken Toe
- Throbbing pain
- Swelling
- Bruising on the skin and toenail
- The inability to move the toe
- Toe appears crooked or disfigured
- Tingling or numbness in the toe
Generally, it is best to stay off of the injured toe with the affected foot elevated.
Severe toe fractures may be treated with a splint, cast, and in some cases, minor surgery. Due to its position and the pressure it endures with daily activity, future complications can occur if the big toe is not properly treated.
If you have any questions please feel free to contact our office located in Pembroke Pines and Plantation, FL . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
What to Know About a Broken Toe
Trauma to the foot, especially the toes, can occur in many ways. Banging them, stubbing them, or dropping something on them are a few different ways this trauma can occur. Given the fact that toes are positioned in front of the feet, they typically sustain the brunt of such trauma. When trauma occurs to a toe, the result can be a painful break or fracture. Another type of trauma that can break a toe is repeated activity that places stress on the toe for prolonged periods of time.
Broken toes can be categorized as either minor or severe fractures. Symptoms of minor toe fractures include throbbing pain, swelling, bruising on the skin and toenail, and the inability to move the toe with ease. Severe toe fractures require medical attention and are indicated when the broken toe appears crooked or disfigured, when there is tingling or numbness in the toe, or when there is an open, bleeding wound present on the toe.
Generally, a minor toe break will heal without long-term complications. However, it is important to discontinue activities that put pressure on the toe. It is best to stay off of the injured toe and immediately get a splint or cast to prevent any more additional movement of the toe bones. You can also immobilize your toe by placing a small cotton ball between the injured toe and the toe beside it. Then, tape the two toes together with medical tape. Swelling can be alleviated by placing an ice pack on the broken toe directly as well as elevating your feet above your head.
Severe toe fractures may be treated with a splint, cast, and in some cases, minor surgery, especially when the big toe has been broken. Due to its position and the pressure the big toe endures with daily activity, future complications can occur if it is not properly treated. Pain associated with minor toe fractures can be managed with over-the-counter pain medications. Prescription pain killers may be necessary for severe toe fractures.
The healing time for a broken toe is approximately four to six weeks. In severe cases where the toe becomes infected or requires surgery, healing time can take up to eight weeks or more. While complications associated with a broken toe are immediately apparent, it is important to note that there are rare cases when additional complications, such as osteoarthritis, can develop over time. You should immediately speak with your podiatrist if you think you have broken your toe due to trauma. They will be able to diagnose the injury and recommend the appropriate treatment options.
What Causes an Ingrown Toenail to Become Infected?

An ingrown toenail occurs when the edge of the toenail grows into the surrounding skin causing pain, redness, and swelling. This condition typically affects the big toe, although it can occur on any toe. Ingrown toenails are often caused by improper nail trimming, where nails are cut too short or rounded at the corners. Wearing tight-fitting shoes that apply pressure on the toes can also contribute to the problem. In some cases, trauma or injury to the toenail can lead to an ingrown toenail. The nails can become infected when left untreated, leading to increased pain, pus, and inflammation. Infection occurs when bacteria enter the broken skin surrounding the nail, causing the area to become swollen and tender. If you have an ingrown toenail, it is suggested that you consult a podiatrist who can offer effective treatment options that may keep it from getting infected.
Ingrown toenails may initially present themselves as a minor discomfort, but they may progress into an infection in the skin without proper treatment. For more information about ingrown toenails, contact Daniel Bell, DPM of Florida. Our doctor can provide the care you need to keep you pain-free and on your feet.
Ingrown Toenails
Ingrown toenails are caused when the corner or side of a toenail grows into the soft flesh surrounding it. They often result in redness, swelling, pain, and in some cases, infection. This condition typically affects the big toe and may recur if it is not treated properly.
Causes
- Improper toenail trimming
- Genetics
- Improper shoe fitting
- Injury from pedicures or nail picking
- Abnormal gait
- Poor hygiene
You are more likely to develop an ingrown toenail if you are obese, have diabetes, arthritis, or have any fungal infection in your nails. Additionally, people who have foot or toe deformities are at a higher risk of developing an ingrown toenail.
Symptoms
Some symptoms of ingrown toenails are redness, swelling, and pain. In rare cases, there may be a yellowish drainage coming from the nail.
Treatment
Ignoring an ingrown toenail can have serious complications. Infections of the nail border can progress to a deeper soft-tissue infection, which can then turn into a bone infection. You should always speak with your podiatrist if you suspect you have an ingrown toenail, especially if you have diabetes or poor circulation.
If you have any questions, please feel free to contact our office located in Pembroke Pines and Plantation, FL . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Ingrown Toenails
Ingrown toenails (onychocryptosis) are a common foot ailment and it is very unpleasant to experience. The condition is caused by an increase in pressure from the ingrowth of the nail edge into the skin of the toe. Ingrown toenails commonly cause pain in those who experience them. In some cases, the skin surrounding the ingrown toenail may break which may lead bacteria to enter through and cause an infection. Common symptoms of this ailment include pain, redness, swelling, and warmth around the toe.
An imbalance between the size of the nail and the enlargement of the nail skin edge causes ingrown toenails. This condition is often caused by improperly trimming the toenails. If you are trying you cut your nails, you should always try to trim straight across instead of in a rounded shape. Ingrown toenails can also be an inherited condition and they may also be caused by improper shoe fitting.
Another common cause of the condition is wearing shoes that are either too small or too large. Other causes include poor foot hygiene, obesity, diabetes, arthritis, edema, and fungal infections. There are many risk factors that may make a person more likely to develop an ingrown toenail. Athletes who play “stop and start” sports such as tennis, soccer, and basketball are most likely to have ingrown toenails.
People who have diabetes, a compromised immune system, or poor circulation should immediately seek care from a podiatrist if they have an ingrown toenail. It is also recommended to seek professional assistance if at-home remedies are not successful within a week or if there is persistent pain.